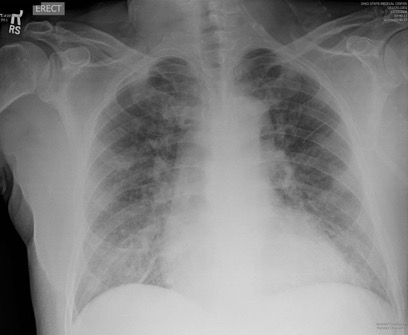
Given these changes from the original case, what is your diagnosis?
What is your diagnostic explanation?
As compared to the long case, this patient is a 62-year-old man who presents to clinic (at the urging of his wife) with exertional dyspnea. He becomes winded after climbing a single flight of stairs. He also reports a cough, which he has noticed for approximately the past month; on further questioning he states that it has been intermittent over the past 2-3 years. The cough is productive of plentiful amounts of whitish-yellow sputum. No hemoptysis. No chest pain. No fever/chills. He presented to convenient care several months ago with a similar cough, where he was given azithromycin. He is a current smoker with a 40-year pack history. He used to enjoy evening walks with his wife, but no longer exercises due to progressively worsening dyspnea. On exam the patient appears obese, calm, alert, oriented and in no obvious distress. Temperature is 37C, HR 96, BP 120/76, RR 20. Breath sounds are distant on auscultation. Expiration is notably prolonged. End-expiratory wheezes are heard. The chest wall is hyperresonant to percussion.